'Five years and $20,000': The real cost of IVF
By Nicola Field
In the time it takes for you to read this article, 11 newborns will have made their way into the world across Australia. Close to 300,000 babies are born annually around the nation, making pregnancy and childbirth a commonplace event. What's extraordinary is that one in 20 of those babies relied on in vitro fertilisation (IVF).
Forty years ago, Australia was an IVF pioneer. Today IVF and assisted reproductive technology (ART) are big business, supporting a wide variety of private clinics, many of which are owned by publicly listed companies.
These companies have followed the money trail. IVF is not cheap and it's not widely available through the public health system. The cost varies between private clinics, but as a guide expect to pay around $220 to $350 for a first consultation. From there, an initial IVF cycle can cost $8680. After allowing for a Medicare rebate and Medicare safety net (more on this later), the likely out-of-pocket cost to the patient can be about $3800.
These figures may be base estimates only. For couples relying on intracytoplasmic sperm injection (ISCI), which can be used to assist with male infertility, the cost of an initial cycle can rise to $9560, with the out-of-pocket expense likely to be in the order of $4200.
The real clincher is that it can take multiple cycles to fall pregnant. According to the Victorian Assisted Reproductive Treatment Authority (VARTA), most people who go through IVF, regardless of age, do not have a baby after just one cycle.
A 2020 report by the UNSW, found that in 2018, over 84,000 IVF cycles were initiated Australia-wide. Yet in that same year, only 14,355 IVF babies were born. That's about a 16% success rate. In reality, success rates vary significantly, and while infertility is a complex issue, a critical factor can be a woman's age.
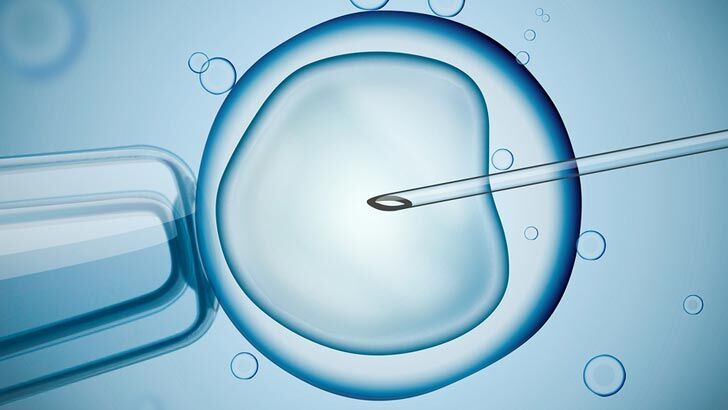
How many cycles?
As the table (IVF success rates) shows, a woman under 30 has close to a one-in-two chance of getting pregnant on the first round of IVF.
That can rise to almost seven out of 10 after three cycles.
However, by the time a woman is in her mid-40s, she faces a near-zero prospect of pregnancy even with IVF.
As Your Fertility, a coalition of fertility experts notes, both men and women experience a natural decline in fertility as they age.
Not even the technology involved with IVF can compensate for this. That said, VARTA points out that if a woman in her 40s uses eggs donated by a younger woman, she faces the same odds as a woman the age of the donor.

No guarantee of success
These figures can fuel the view that IVF is a numbers game - the more cycles you have, the greater the odds of falling pregnant. But nothing is set in stone.
For Alice Almeida, who was diagnosed with endometriosis in her early 30s, it took five years and four cycles of IVF before she gave birth to her now three-year-old daughter.
That was followed by three more unsuccessful attempts to have a second child through IVF.
"IVF is one of the few industries where you pay but there is no guarantee you will get the end product - a baby," says Almeida.
"It is critical for people to realise that IVF gives you a chance of a baby, but there are no guarantees of success."
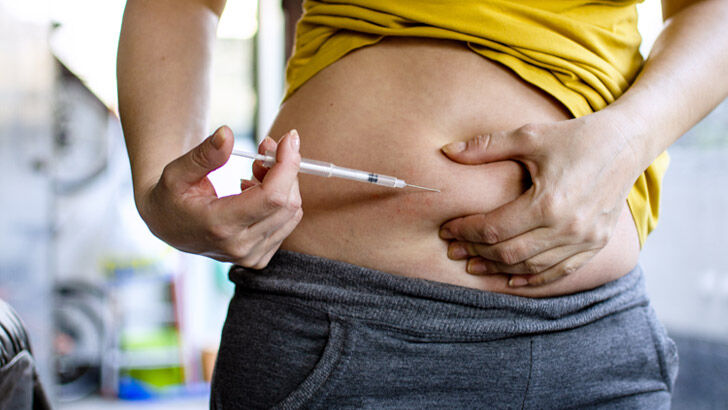
What it can cost
For couples and women about to embark on an IVF journey, there are options to manage the cost.
In NSW, the state government has expanded the availability of lower-cost IVF treatment at three publicly supported IVF clinics: the Royal Prince Alfred Hospital, the Westmead Fertility Centre and the Royal Hospital for Women.
At Westmead, for example, an IVF cycle, including embryo freezing, three months' storage and day surgery, can now cost only $1000.
In Victoria, the Royal Women's Hospital is one of the few places that makes low-cost IVF available.
Some private clinics, such as Adora Fertility, provide Medicare bulk billing so patients only pay for services not covered by Medicare. This can include day surgery and anaesthetist fees for egg collection, along with some medications.
Private health cover can help with the cost of IVF. If you're relying on health insurance, check the services you're covered for and, importantly, whether you have completed any required waiting periods.
Infertility can be seen as a pre-existing condition and that means a 12-month waiting period may apply before claiming benefits.
If your current policy doesn't include "assisted reproductive services", you'll likely need to upgrade your policy. Even with health cover, you could face a gap fee. Egg collection, for example, is a surgical procedure and there can be a shortfall between the fees charged by your anaesthetist and doctor and the amount you're covered for.
The Commonwealth Ombudsman recommends getting a detailed quote from an IVF clinic, including all medical item numbers, and asking your health fund what is - and is not - covered.
Beyond this, some costs can be claimed through Medicare as well as the Medicare safety net, which provides an additional capped rebate once you reach a certain amount of medical expenses per calendar year. The safety net is not means-tested, and there are no restrictions on the number of IVF cycles you can go through each year.
Nonetheless, be prepared to dig deep.
"We have private health cover, however only hospital visits were covered," says Almeida. "Our out-of-pocket costs were partly covered by Medicare. But we still ended up paying close to $5000 per cycle because the medication women are required to take as part of IVF is very expensive."

Expect the unexpected
While clinics are upfront about the costs of egg collection, fertilisation and storage of embryos, IVF can bring a raft of unexpected bills.
"The medications, the cost of genetically testing each embryo - it's not a one-off payment," says Almeida. "You are paying constantly. You are so desperate to have a baby that you agree to the tests and think about the financial side later. Before you know it, you've paid $20,000."
The overwhelming drive to have a baby can see people pay for alternative fertility treatments that may have dubious rates of success.
"IVF is not just about the science. You become so desperate for a baby you will try anything," says Almeida. "I spent $2000 on Chinese medicine. Along with acupuncture, a naturopath, a fertility coach and 'IVF yoga' classes, I spent as much outside the clinic as I did on IVF."

How to pay for it
Part of the challenge of paying for IVF is that infertility can come as a surprise. It's not something we tend to put savings aside for.
Private clinics may offer payment plans that spread the cost over time. Many feature online links to SuperCare, which charges IVF patients a fee to access their super early to pay for treatment - a process that you can potentially do yourself at no cost.
A number of smaller lenders, such as Jacaranda Finance and Harmoney, promote medical loans that can be used to fund IVF. These are essentially unsecured personal loans, so it's worth shopping around, though not all mainstream banks will lend for IVF treatment.
Overriding this is the uncertainty of how many cycles it may take to fall pregnant, which makes it hard to plan ahead financially. If a pregnancy does result, additional resources will be needed to pay for the newest family member.
The upshot is that IVF can bring a solid financial burden.
"All up we spent around $50,000 to have our baby - the deposit for our dream home," says Almeida. "But we are among the lucky ones. People save for years for IVF and still don't have a baby."

When employers help with the cost
It won't appeal to every woman, but employer-sponsored egg freezing is fast becoming a work perk. It was introduced in the US as far back as 2014 by corporate giants Apple and Facebook. Around one in five large US companies now offers female employees financial support to access egg freezing, with predictions Australia could follow suit.
It can certainly provide financial relief. At IVF Australia, for instance, egg freezing costs $4490 plus $1500 for the required medications. Storage costs can be $500 annually.
A Monash University study found almost half the Victorian women surveyed were comfortable with the idea of the boss paying for egg freezing.
Ultimately, egg freezing is an expensive procedure that is only partially supported through Medicare, meaning many women may not be able to access the procedure because they cannot afford the costs," says Molly Johnston, from the Monash Bioethics Centre.
"Or they are freezing their eggs at an older age when they can afford the procedure, but it is less effective and the chances of achieving a live birth are significantly reduced.
"Employer-sponsored egg freezing could enable young female employees, who might not be ready to have a child, access fertility preservation. It could be seen as a win-win for employers and employees."

Success rates vary
It's fair to say many couples will select an IVF clinic based on the prospects of success rather than cost. A 2016 investigation by the Australian Competition and Consumer Commission found clinics were using a variety of measures of success rather than live births.
Stirling Griff, a senator for South Australia, has been an advocate for change on this score and pushed for the launch of YourIVFSuccess, a new website that shows the percentage of embryos transferred that lead to a live birth for each clinic, and compares this to national rates.
"The website means infertile Australians will no longer be flying blind when they choose a clinic," says Griff.
"They can use the website to research and view the performance of each fertility clinic."
YourIVFSuccess also includes an IVF success estimator, which Griff says lets "those thinking about starting or continuing IVF make informed decisions".
However, as an IVF veteran, Almeida sees some shortcomings.
"I entered my own details in YourIVFSuccess (from when I started IVF) and it came up with a 29% chance of success," she says.
"Yet after eight embryos were transferred, only one led to a baby. The website is not sufficiently personalised for individual women. This creates the risk that it could create false hopes or, alternatively, stop people on their IVF journey."

When to start ... or quit
As challenging as it may be, Almeida recommends going into IVF with a realistic mindset.
"Seeing a financial planner can help you understand how to meet the costs of IVF. This is important as financial decisions shouldn't be made on desperation and emotions."
The hardest part, however, for many women or couples may be knowing when to draw a line in the sand. Research confirms some couples keep going with IVF for multiple cycles, despite limited chances of success.
One message is clear: don't leave things too late.
"Fertility potential can vary greatly from your mid-30s onwards," cautions Manuela Toledo, medical director at TasIVF, a fertility clinic in Hobart. "The ideal time to connect with a fertility specialist is in your early 30s to discuss future fertility planning such as elective egg freezing.
"If you've reached the age of 35 and you're not quite ready to have a baby, or you can't see a baby on the horizon just yet, that's the time to see a fertility specialist to discuss your options and to have an individualised fertility assessment."
If you're thinking about egg freezing, Toledo says "the best time to freeze your eggs is at your peak fertility, which is in your 20s and early 30s. Generally, in this age range the eggs are still plentiful and in good quality, so it becomes more cost-effective as the pregnancy potential per egg is at its highest."

Mental health is important
As a result of her IVF experience, Alice Almeida has recently launched the Amber Network, a web-based hub for both men and women going through infertility and IVF.
It's aimed at giving people a better idea of what they're about to go through, with a focus on mental health and self-care.
"IVF clinics don't address mental health anywhere near enough - it's often treated as an after-thought," says Almeida. "I was entitled to one free counselling service with my clinic, but any other counselling came with additional cost."
The website features a community section that allows people to connect, if they wish, with others opting for IVF, plus a list of relevant services.
Get stories like this in our newsletters.



